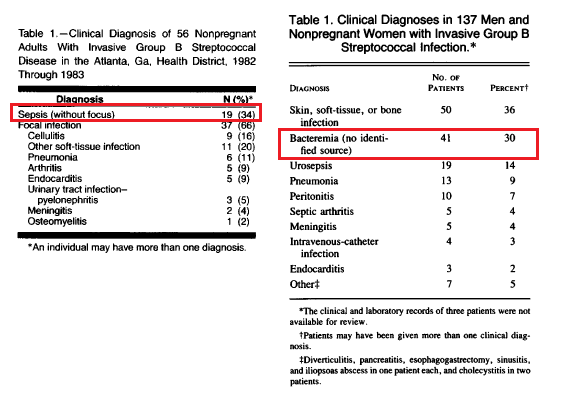
The rate of invasive group B streptococcal infection has been rising for the past few years. Originally described in neonates and pregnant woman, the incidence of invasive disease has risen significantly in the non-pregnant adults. Early studies (1, 2) from Atlanta in the early 90s found that in non-pregnant adults, bacteremia without a focus and SSTI were common disease manifestation of GBS, with an annual incidence of 4.4 per 100,000 in this population:

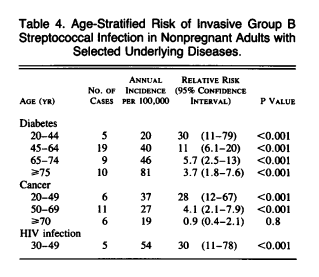
Further data (2) also found that advanced age, diabetes, and HIV status were significant risk factors for GBS:
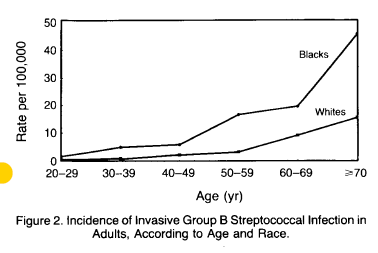
And, I guess I should say, not surprisingly, African Americans were twice as likely to have invasive GBS infection (6.5 per 100,000 in AA, 3.2 per 100,000 in White). Further, those people residing in Fulton Count (which includes the urban center of Atlanta) had a RR of invasive GBS infection of 2.9 when compared to the 7 other counties.
Smaller (3) data from Argentina found that in 1110 bacteremic episodes, 13 of those were with GBS. In 5 of those cases, patients presented without a focus. A larger Korean (4) retrospective analysis of 103 GBS bacteremic patients found that advanced liver cirrhosis is associated with a significantly higher mortality and while, not significant, alcohol abuse tended to be found more commonly in those who had died:

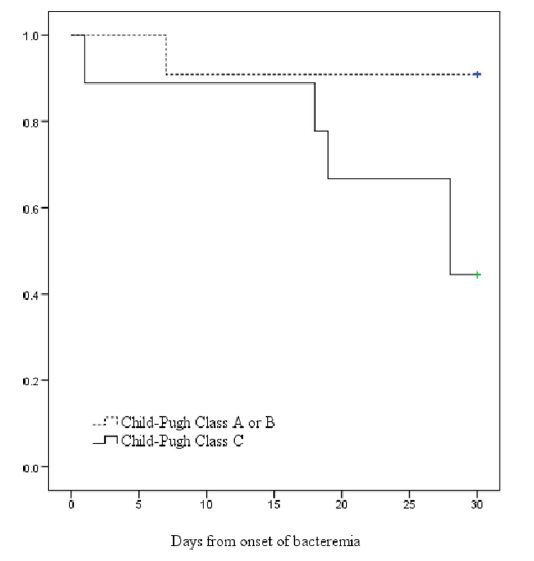
Those with worsening liver failure fared worse in terms of mortality. Mortality increased from 0%, 16.7%, and 83.3% in CP classes A, B, and C respectively (p-value 0.035).
The 30 day survival was worse in those with Childs-Pugh Class C (HR 8, 95% CI 2.44-26.3, p-value 0.001).
A few more recent studies have confirmed the pattern of invasive disease. For instance, a French (5) retrospective analysis found that most patients presented with bacteremia without a focus and SSTI:
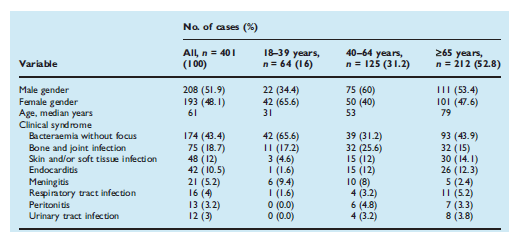
While most of the data above is older or from smaller datasets, the following 2 population-based surveillance data seems to corroborate the rising incidence of invasive GBS. For instance, using the Active Bacterial Core surveillance (ABCs) network, 21,250 cases of invasive GBS in non-pregnant adults were found between 2008-2016 (6). They note the incidence in all ages increased from 8.1 to 10.9 cases per 100,000 between this time period:
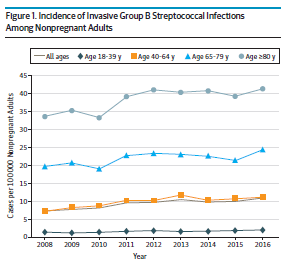
They further note that Blacks had a higher incidence overall, but the difference waned by 2016. Further, patients with obesity, T2DM, and heart failure accounted for a significant percentage of those patients with invasive GBS.
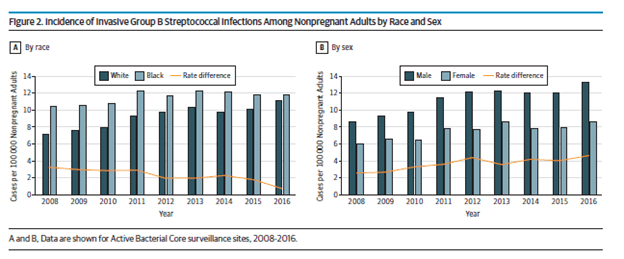
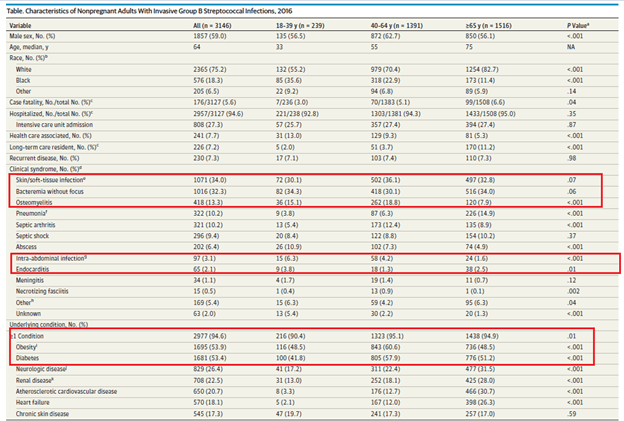
A few things to highlight from the above table:
- Again, roughly 30-36% of patients present with SSTI while bacteremia without a focus accounts up to 34% of patients.
- Intra-abdominal infection, interestingly, does not account for a significant portion of cases
- Endocarditis, at least in this cohort, was a small percentage
- Obesity and diabetes were seen in a majority of those with invasive GBS
A retrospective study from England (7) evaluated 3156 episodes of invasive GBS. The incidence, once removing 479 episodes of pregnancy related GBS, was 2.9 cases per 100,000. As noted before, the incidence tended to go up with age, although there was a prevalence of cases in those aged 30-39, mostly due to female and pregnancy cases.
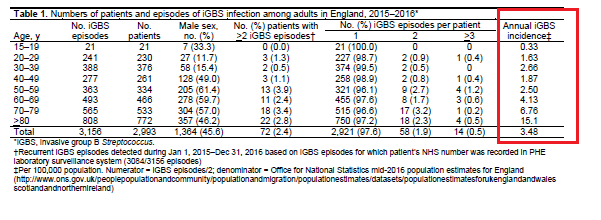
This retrospective study also found that lower socioeconomic status was more prevalent in those with GBS:
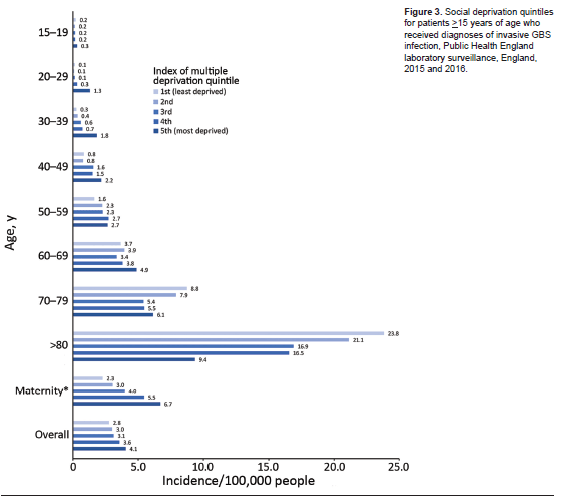
All-cause 30 day mortality was 12.5%, with the number extending up to 29% at 12 months. Main driver here was co-morbid conditions (OR 5.3, 95% CI 1.7-16.9), older age (OR 3.7% 95% CI 1.5-9.3 when compared to those aged 20-29)

A more recent cohort study (8) from the VA evaluated GBS in 5497 (mostly white male) patients. In this cohort, most of the invasive GBS was in the form of osteomyelitis (21.3%), followed by bacteremia without a focus (18.4%), and SSTI 16.7%):
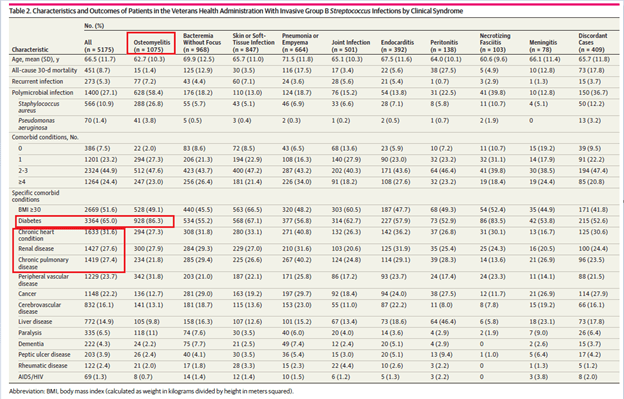
The more common co-morbidities found were diabetes, heart disease, renal disease, and pulmonary disease. Overall, mortality range from 1.4% in osteomyelitis to up to 27.5% in peritonitis, 17.5% in pneumonia/empyema, and 12.9% in bacteremia:
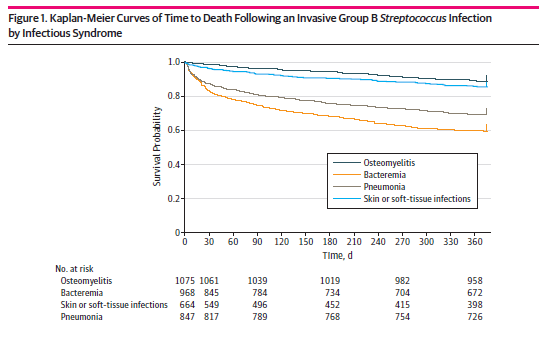
Another thing to point out with regards to the above studies is the overall mortality. 30d mortality tends to range from 3% in younger patients up to 21% in male patients >80 and up to 43.7% in female patients >80. In the above mentioned Korean study (4), the mortality for those patients without liver cirrhosis was 8% and went up to 26% in those with liver cirrhosis and the type of invasive disease also tends to matter, with bone, joint, and skin/soft tissue infections having less mortality when compared to bacteremia without a source.
TL;DR
- Group B strep is a rising etiology of invasive disease
- RF include liver disease, diabetes, heart disease
- It is not unusual to find bacteremia without a source here. Having said that, look for a cellulitis or skin/soft tissue infection and if someone has any localizing pain, it may be helpful to look for that bone infection
- Elderly age and liver cirrhosis tends to portend a poor prognosis.
References:
- Schwartz B, Schuchat A, Oxtoby MJ, Cochi SL, Hightower A, Broome CV. Invasive Group B Streptococcal Disease in Adults: A Population-Based Study in Metropolitan Atlanta. JAMA. 1991;266(8):1112–1114. doi:10.1001/jama.1991.03470080082034
- Farley MM, Harvey RC, Stull T, et al. A population-based assessment of invasive disease due to group B Streptococcus in nonpregnant adults. N Engl J Med. 1993;328(25):1807-1811. doi:10.1056/NEJM199306243282503
- Saad, Emanuel J., et al. “Streptococcus Agalactiae Bacteremia in Non-pregnant Adult Patients at Two Teaching Hospitals.” Revista Argentina De Microbiologia, vol. 50, no. 3, 2018, pp. 280-284.
- Park SY, Park Y, Chung JW, et al. Group B streptococcal bacteremia in non-pregnant adults: results from two Korean centers. Eur J Clin Microbiol Infect Dis. 2014;33(10):1785-1790. doi:10.1007/s10096-014-2140-9
- Tazi, A, et al. “Invasive Group B Streptococcal Infections in Adults, France (2007-2010).” Clinical Microbiology and Infection : the Official Publication of the European Society of Clinical Microbiology and Infectious Diseases, vol. 17, no. 10, 2011, pp. 1587-9.
- Francois Watkins, Louise K., et al. “Epidemiology of Invasive Group B Streptococcal Infections Among Nonpregnant Adults in the United States, 2008-2016.” JAMA Internal Medicine, vol. 179, no. 4, 2019, pp. 479-488.
- Collin, Simon M., et al. “Invasive Group B Streptococcus Infections in Adults, England, 2015-2016.” Emerging Infectious Diseases, vol. 26, no. 6, 2020, pp. 1174-1181.
- Jump RLP, Wilson BM, Baechle D, et al. Risk Factors and Mortality Rates Associated With Invasive Group B Streptococcus Infections Among Patients in the US Veterans Health Administration. JAMA Netw Open. 2019;2(12):e1918324. doi:10.1001/jamanetworkopen.2019.18324